Two things are happening in parallel that don't usually happen at the same time. Employer medical and pharmacy trends are running hot enough that more than a third of employers are actively in-market with RFPs right now. And OPM has quietly, but firmly, elevated digital therapeutics and "well care" to a stated carrier priority, pulling behavior change back onto the federal agenda for the first time in years.
That convergence is not incidental. It is a rare window for benefits consultants to reframe behavior change programming, not as a participation point perk, but as a measurable lever on medical and pharmacy trend. The caveat: only a real behavior change program can hold up that reframe. A nudge app cannot.
Why the "perk" frame has outlived its usefulness.
Wellness programs inherited their reputation from the points and gift cards era. The framing was engagement first and CFO optional. That has been quietly costing consultants credibility in risk and finance conversations, because "engagement" loses every time it meets a dollar sign. When the business case is reframed, moving tobacco, obesity prep, hypertension, and depression adherence with trial evidence behind it, it competes.
The "behavior change" label has also been diluted. The category is crowded with products marketing themselves as behavior change when they are really reminders, streaks, and points stacked on a gamification layer. A nudge can change a moment. A real behavior change program, grounded in cognitive behavioral training, shaped by decades of clinical practice, delivered by trained content experts and certified coaches, and evidenced in controlled trials, changes the underlying response to a habit. Those are different products, and consultants need to be able to tell them apart for a client on a single page.
What the OPM signal actually means.
Federal employee benefit priorities tend to move slowly and then all at once. OPM's elevation of digital therapeutics and well care is not a mandate for commercial plans, but it functions as credibility cover. When a consultant tells a self-insured employer that the federal government is now treating behavior change as a cost containment tool, that conversation lands differently than it did two years ago.
It also signals where the carrier market is heading. Commercial carriers read OPM priorities. The consultants who get ahead of this frame now will be better positioned when carriers start leading with it themselves.
How to tell a real program from a nudge app.
The category confusion is real and it costs consultants credibility when a client's previous "behavior change" program was just a points app. Here is a one-page test:
A real behavior change program has a clinical foundation (cognitive behavioral training, not gamification), structured course content built by credentialed experts, 1-to-1 coaching by certified professionals, and outcome data from controlled studies. It targets specific conditions, including tobacco use, weight management, alcohol, stress, and sleep, with course content matched to each. A nudge app has a streak counter and a leaderboard.
The distinction matters in an RFP because outcomes language is only defensible if the program can actually produce outcomes. A tobacco quit rate of 38.1% at six months post-completion, from a controlled San Diego State University study, is a number a CFO can underwrite. "Participants felt more motivated" is not.
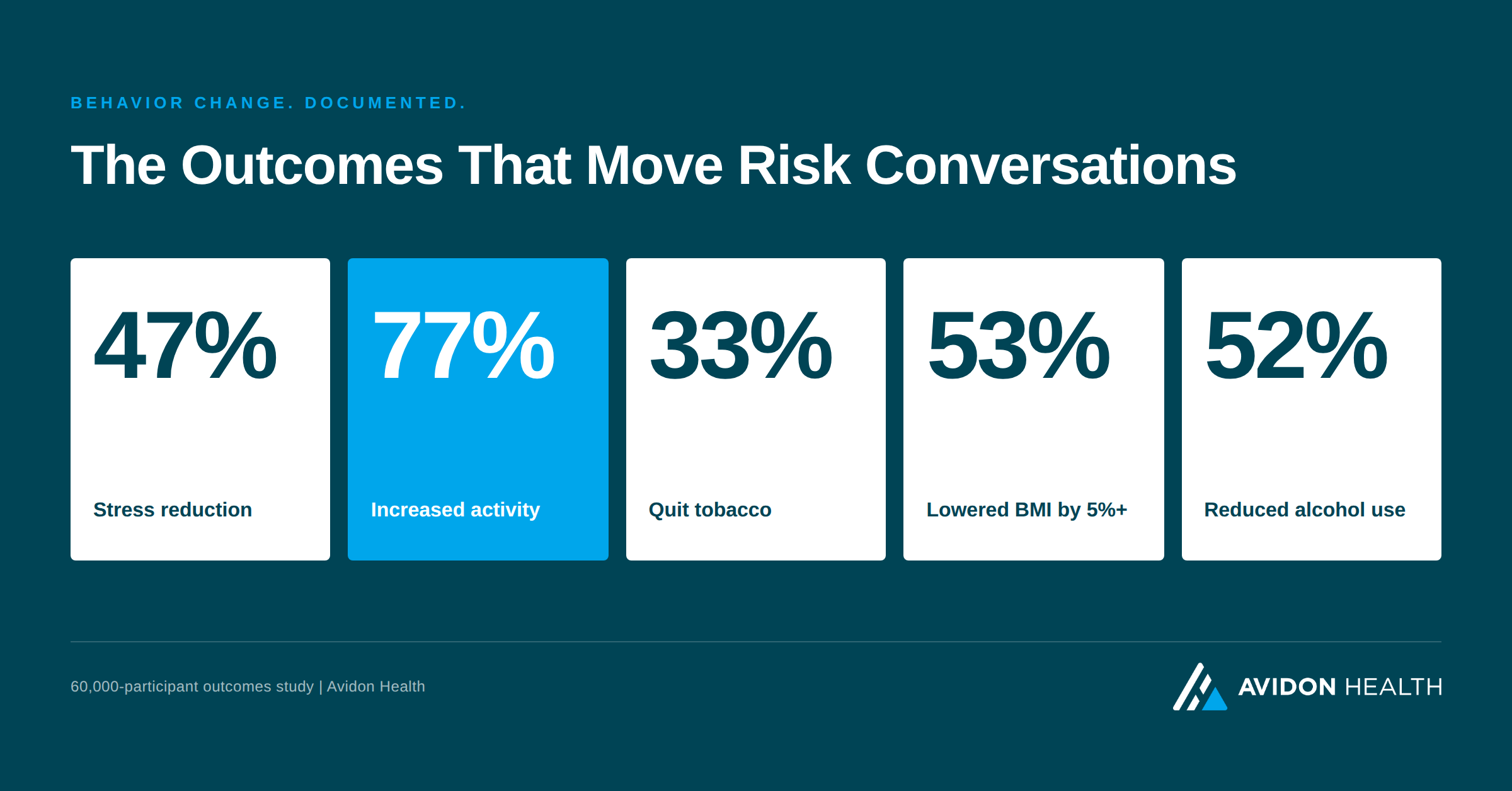
The proof points that move risk conversations.
Three data points tend to shift the conversation in employer risk reviews:
The GLP-1 adherence angle: behavior change programming addresses the lifestyle scaffolding that determines whether a GLP-1 investment holds. Without it, the drug's ROI erodes. With it, the employer is protecting a significant pharmacy spend. That framing resonates with any CFO currently staring at a GLP-1 line item.
The tobacco quit rate: 38.1% at six months in a controlled trial. Tobacco is still one of the highest-cost, most addressable drivers of employer health spend. A documented quit rate is one of the cleaner ROI calculations in the benefits stack.
Where this fits in the RFP conversation.
The right moment to introduce the behavior change reframe is not the wellness section of the RFP. It is the medical and pharmacy trend section, where the client is already talking about cost. Framing behavior change as a clinical complement to disease management and pharmacy spend, not as a culture-and-engagement add-on, changes which decision-makers are in the room and how the budget conversation goes.
The consultants getting traction with this frame right now are leading with outcomes, naming the conditions they can move, and letting the OPM signal do some of the credibility work. The window is open. The question is whether the program you're recommending can hold up the claim.